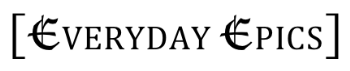Although the U.S. Supreme Court declared the Patient Protection and Affordable Health Care Act constitutional late last month, the fate of the act still depends in large part on the outcome of this November’s national elections. And while some of its provisions have already taken effect in Colorado and elsewhere, it is unclear if the Act will adequately address the barriers faced by some children and adults living outside the health care system.
Uninsured children
Dr. James Todd, the director of epidemiology, clinical outcomes and clinical microbiology at Children’s Hospital Colorado in Aurora, Colo., co-authored a 2006 paper in the journal Pediatrics. Its title: “Increased Rates of Morbidity, Mortality, and Charges for Hospitalized Children With Public or No Health Insurance as Compared With Children With Private Insurance in Colorado and the United States.”
Todd says from his small fourth floor office at Children’s Colorado, “The sad thing is that not much has changed since we published the paper back in 2006. We have found anywhere from 25-50 percent or more of the kids discharged didn’t have health insurance before they came in.”
“Over the last 10 years, the number of kids on private insurance has decreased and the percentage of children who are on public or no insurance has gone up. We can say that there are relatively persistent disparities in outcome – fatality rates are higher in the no or public insurance group, hospitalization rates are significantly higher, admission through the emergency department is significantly higher…We’ve found the same for pregnant women. There is a decreased access to prenatal care for those with public and no insurance, and a higher morbidity rate. There are disparities and in many circumstances they’re getting worse.”
For example, a child who complains of lower abdominal pain soon sees her regular pediatrician if her parents have private insurance. The pediatrician diagnoses her symptoms, say, as appendicitis, and admits the child to the hospital for a one-day stay. She gets treated and recovers quickly. However, if she or her parents have no insurance or public insurance, she goes without immediate care, her appendix ruptures and she is forced to stay in the hospital for one to three weeks to recover.
Those kinds of “excess admissions” are preventable, Todd says. “Not being eligible is a bad thing, but if you’re eligible and you don’t have a doctor, that’s not good enough. Being eligible isn’t being enrolled. Being enrolled doesn’t mean you have adequate access to a medical home. And what you really need is a medical home.”
According to Todd, practices that decrease the disparity in health care access and outcomes include increasing Medicaid enrollment, improving vaccination rates and increasing kids’ access to primary medical care.
In 2006, due to extremely low reimbursement rates, only 22 percent of Colorado pediatricians and family physicians accepted Medicaid or Child Health Plan Plus (CHP+), the two main health insurance programs for low-income families and children.
“The [reimbursement] rate was so low that physicians lost money on every patient they saw,” Todd says. “You can’t keep a private practice open if you’re losing money on every patient you see.”
To address physician’s barriers to participating in government-funded programs and provide children with a medical home, the Colorado Children’s Healthcare Access Program (CCHAP) began in 2006 under the direction of Dr. Steven Poole, one of the co-authors of the above-cited article in Pediatrics. While 95 percent of Colorado’s private pediatric practices had affiliated with CCHAP as of 2010, Todd says about 125,000 children in Colorado still do not have health insurance.
“Shouldn’t every child be eligible for health care, enrolled in a health care insurance program and have access to affordable primary medical care?” Todd asks. “Well, people ask, ‘Who’s going to pay for that?’ People say ‘When it comes down to my tax rate, I want lower taxes,’ but I’m asking, ‘Even if that means we have 125,000 children in Colorado who don’t have health care or we have millions of children nationwide without health care insurance?'”
Uninsured adults
The federal and state governments fund Community Health Centers (CHCs) in areas where the income of enough people falls below the federal poverty threshold. Along Colorado’s Front Range, 11 CHCs with specific geographical boundaries, provide free or low-cost medical care to local residents. For example, Denver Health is a CHC and a network that provides hospital access and clinic services for low-income residents of the City and County of Denver.
The level of federal funding a CHC receives depends on its number of Medicaid patients, which currently includes children under 18, pregnant women and people who are disabled.
“I have one patient whose son was disabled by a horrible car accident, and she was too,”
says Dr. Annie Dominguez, a bilingual physician at Salud Family Health Center in Commerce City, Colo. “She is not old enough for Medicare. She, her husband and her son live in a trailer…She is on our sliding fee scale, and I see her twice a year. They live off the Social Security her husband gets from being retired…They go to two food banks in Commerce City, and choose whether they’re going to pay for seizure medications or diapers for their disabled son.”
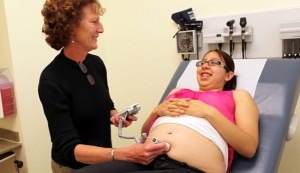
Some Colorado residents, however, are not eligible even to receive care on a sliding scale at a CHC, including low-income residents who live in rural or relatively well-to-do areas outside CHC boundaries, low-income adults who live outside Denver but need non-emergency hospital care, and undocumented adults and children. (Colorado House Bill 06S-1023, enacted on July 31, 2006, allows state public benefits to go only to lawful residents of Colorado.)
Many of these ineligible residents end up in an emergency room when they need medical care. Often times they have no health insurance. As a result, they are billed at a far higher rate than if they had insurance. When they can’t pay, they get hounded by creditors so they change their phone number, move somewhere else and leave no forwarding address, or they otherwise start to give false information when they have contact with the system.
Among the few local institutional alternatives for adult patients who are ineligible to use area CHCs is the faith-based Inner City Health Center (ICHC) on York Street and 38th Avenue in Denver, Colo.
“There are always people falling through the cracks,” says Dr. Bob Cutillo, the ICHC’s medical director. “There is a real underside of the health care system.”
ICHC relies on the help of physician volunteers, but still faces an ongoing budget shortfall. “We’re funded by patient fees, foundation grants, individual churches, personal donors, corporate support, and some money from the State of Colorado,” he says. “We want to create a haven for people in need, but honestly in our current climate we’re losing $25,000 per month.”
ICHC uses a sliding scale for its patient fees, but in order to qualify for its income-based discount, patients must provide proof of income or a W-2 form. A pregnant woman, for example, pays about $350 for 10 prenatal visits and an ultrasound.
“For uncomplicated care that [fee system] is adequate, but you’re in big trouble if you have a major health issue,” Cutillo says, noting his reliance on a small, informal network of physicians to donate their time so his patients can have necessary surgical procedures. “People still think of health care as a possession, not a community-oriented societal good, but people realizing how broken our system is is the beginning of people wanting to change it.”